During the coronavirus pandemic, many countries have effectively banned group singing and playing of woodwind and brass instruments. Although there have been several clusters of Covid-19 noted in choirs around the world, there is no concrete evidence to link these cases to the acts of playing and singing. The University of Bristol, Imperial College London, Wexham Park Hospital, Lewisham and Greenwich NHS Trust, Royal Brompton Hospital and ARUP have all banded under the name PERFORM for a Covid-19 research project to tackle this problem.
PERFORM (ParticulatE Respiratory Matter to InForm Guidance for the Safe Distancing of PerfOrmeRs in a COVID-19 PandeMic), supported by Public Health England, will explore whether singing and playing brass and woodwind instruments produces more respiratory particles than when speaking. These aerosol experts will also be investigating whether venue temperature and size affects the amount of aerosol droplets produced.

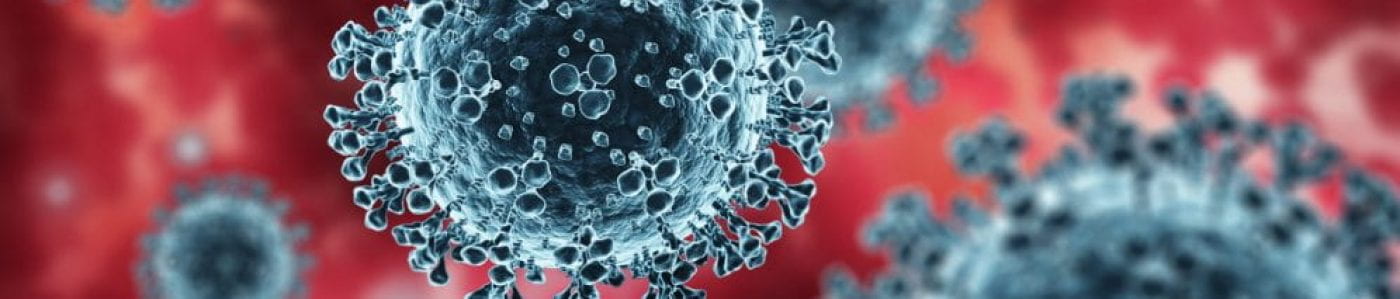
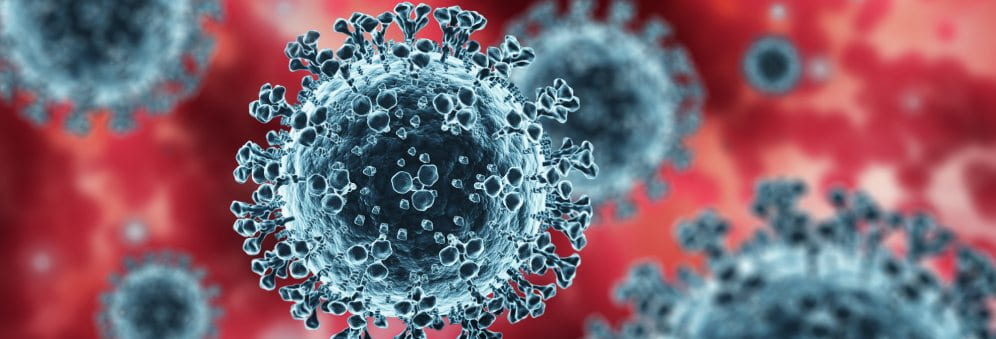
Airborne droplets of a similar diameter to a human hair enable the transmission of the Covid-19 virus through sneezing, coughing, speaking, and even breathing. These droplets can contaminate surfaces up to two metres away that unsuspecting individuals may later touch. And equally troubling are smaller (10 micrometres!), respirable particles that can remain airborne hours after a sneeze, or singing.
Prof. Jonathan Reid from the University of Bristol has been determining whether aerosol droplets could be a culprit in the transmission of the virus. A PERFORM experiment at the University of Bristol includes individuals singing and speaking between the decibel (dB) ranges of 50–60, 70-80 and 90-100 dB. The Langford Vet School and the School of Cellular and Molecular Medicine at Bristol are also exploring how long the virus survives at certain temperatures and relative levels of humidity. They have been in operating theatres working with clinicians to quantify aerosols produced from aerosol generating procedures, such as extubation and intubation.
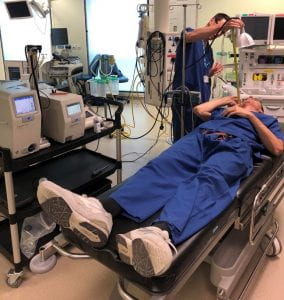
procedures such as extubations.
The results from the Bristol study in conjunction with other outcomes in the PERFORM collaboration efforts against Covid-19 will help to provide more robust evidence for guidance on social distancing, and may provide an answer to the currently uncertain future of choirs and orchestras around the world.